A few months ago, I wrote a post on the neuroscience of vegetative states (read it here). This week, I was completely blown away by Martin’s story reported on NPR’s new show, Invisibilia (listen here). This is a powerful story illustrating the incredible ability of the human brain to change and heal.
Neuroscience
The Brains Are Alive With the Sound of Music
Last weekend I attended a Sound of Music Singalong at the Music Box Theater in Chicago. When I walked through the double doors into the theater, I was given a bag of goodies: plastic Edelweiss to hold up during the song, an invitation to the ball, and a popper that we were instructed to pop when Maria and Captain Von Trapp kissed for the first time. I was struck by the age range of the audience, everyone from graying old ladies to young men to children, with some people even in costume! With the exception of one sullen teenager in a hoodie slouched down in his seat next to me, everyone seemed to be excited. I figured only a couple of extra-enthusiastic people would really sing, so I was pleasantly surprised when Maria came running over the beautiful green Austrian mountain and all my neighbors started passionately belting out “the hills are alive!” Everyone was singing.
I wondered, what is it that compels people of all ages, races and genders to pile into a theater on a Sunday afternoon and sing for over three hours? What is it about music that so inspires and excites people? This is a question that has gripped neuroscientists all over the world, and recent research has started to provide some answers.
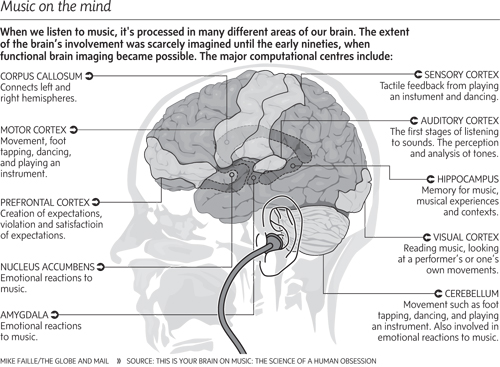
To process music, the nervous system needs to engage a large number of regions starting with the intricate structures in the inner ear, which translate sounds into electrical activity that can be sent into the brain. Neuroimaging work has shown that once the signal enters the brain, it creates widespread neural activity (as seen in the diagram below), resulting in strong emotional responses.
Mysteriously, it has been repeatedly reported that patients with advanced dementia, who may have lost the majority of their long-term memories and even language capabilities, show preserved musical ability and response. It is possible that because of the widespread effects of music on the brain, including areas that are more spared in Alzheimer’s disease, listening to music may be able to awaken and even preserve cognition by accessing memory through alternate pathways.
Can music help dementia patients?
This is the question that Michael Rossato-Bennett addresses in his award winning documentary Alive Inside (available on Netflix streaming). He takes us on the journey of social worker Dan Cohen as he fights a broken healthcare system and illustrates music’s unique ability to fight memory loss in dementia patients. We are told the stories of Henry (see video here) and many other individuals whose responses to music are breathtaking, miraculous transformations from quiet shells into animated characters singing, moving to the beat and tapping into memories going all the way back to early childhood. It provides a gripping view of the unexpected effects of music on patients that were otherwise considered lost to dementia.
As Alive Inside points out, dementia is no small problem. There are 5 million people in America with dementia, and 10 million people spend a large part of their life caring for them. There are maybe a million people in nursing homes, slowly losing their connection to life.
“Music gives us a way to reach someone who may otherwise be unreachable. It creates spontaneity that you cannot create in an institution. It takes you to a place where you can leave and go off to a world that you create and connect with on your own terms. There is no pill that does that.”
And the neuroscience backs this up. In one study done on Alzheimer’s patients, those that listened to “Big Band” music from the 1920’s and 1930’s had better autobiographical memory recall. In another study, Vande Winckel and colleagues showed that when exercise was combined with music (polka, folk and country), mental exam test scores increased and having Vivaldi’s Four Seasons played while taking cognitive tests seems to enhance performance.
Listening to music is a low-cost, noninvasive treatment that has been shown effective in study after study, and it has no side-effects! Yet, this information has not been implemented or utilized on a large scale in nursing homes.
Dan Cohen’s mission is to change that, by bringing personalized music to people suffering from dementia all over the country. When he embarked on this journey in 2006, Dan found that none of the 16,000 long-term care facilities in the U.S. used iPods for their residents. Today Dan’s work has helped provide personalized music programs to hundreds of nursing homes throughout the country. His success demonstrates the power of technology and how it can be used to not only treat symptoms, but deeply connect with a person’s heart and soul to give them back some joy and purpose.
We can still bring life to those people who have been forgotten. We do have something to give. All we have to do is ask, “What is your favorite song?”
Dedicated to my incredibly talented friend Jennifer Mitchell, whose love for music has always inspired me.
References:
“Brain Music.” Brain Music. N.p., n.d. Web. 09 Dec. 2014. <http://www.newswise.com/articles/brain-music>
Lin, Shuai-Ting, Pinchen Yang, Chien-Yu Lai, Yu-Yun Su, Yi-Chun Yeh, Mei-Feng Huang, and Cheng-Chung Chen. 2011. “Mental Health Implications of Music: Insight from Neuroscientific and Clinical Studies.” Harvard Review Of Psychiatry (Taylor & Francis Ltd) 19, no. 1: 34-46.Academic Search Complete, EBSCOhost (accessed December 9, 2014).
Lord TR, Garner JE. Effects of music on Alzheimer’s patients. Percept Mot Skills 1993;76:451–5.
“Our Mission and Vision – Music and Memory.” Music and Memory. N.p., n.d. Web. 09 Dec. 2014. <http://musicandmemory.org/>
Thompson RG, Moulin CJ, Hayre S, Jones RW. Music enhances category fluency in healthy older adults and Alzheimer’s disease patients. Exp Aging Res 2005; 31:91-9.
Van de Winckel A, Feys H, De Weerdt W, Dom R. Cognitive and behavioural effects of music-based exercises in patients with
dementia. Clin Rehabil 2004;18:253–60.
Seeing the light
Imagine being in your early thirties, married and excited about what life has in store for you. One day, you start to notice that your peripheral vision is not as good as it once was. You have a hard time detecting things that are not right in front of you; objects and people start to appear very blurry; reading and driving become impossible. After consulting your doctor about this problem, you are told that you have a genetic condition called retinitis pigmentosa. There is nothing that can be done, and eventually you will lose your sight completely. You will just have to adjust to this new way of life.
In the eye, the cells that convert light signals from the external world into neural signals are called photoreceptors (the rod and cone cells in the diagram below). They sit at the back of the eye and detect light as it hits the retina. Once they detect this light, they have to translate it into a language the brain can understand, crucial for transmitting visual information to the brain. Retinitis pigmentosa causes degeneration of these rod and cone cells, and therefore leads to the breakdown of the interface between the world (light) and the brain. Without these cells, information about a visual scene becomes stuck and unable to get through to the brain to be processed; the brain cannot interpret visual information, eventually leading to blindness.
(Jamie Simon, Salk Institute for Biological Studies)
Larry Hester was diagnosed with retinitis pigmentosa more than 30 years ago, but recently, he was able to see light again for the first time in many years. Researchers at Duke University implanted a device with many tiny electrodes that could essentially bypass the damaged rods and cones to send information to the brain. Here is how it works: Larry wears glasses with a video camera attached, which sends a signal about what Larry is looking at through a tiny wire to a computer attached to his belt. The computer receives the information and relays it to the electrodes on the retina, which activates the cells that project into the brain. The device is translating the light information into neural activity, giving Larry the ability to experience and interpret the image he is looking at. At a basic level, the device is able to perform the function of the photoreceptors that have died.
See Larry’s amazing experience here: http://www.wimp.com/bioniceye/
It is important to note that this technology is new and limited, giving Larry only a blurry version of the world. Despite this, I have no doubt that the technology and its use will continue to improve rapidly, inching closer and closer to giving people normal vision. Larry says it is his dream to be able to see his wife’s blue eyes again. Although he is not able to achieve this with his current implant, at least he is one step closer.
Dr. Paul Hahn, an Assistant Professor at the Duke Eye Center, points out that we are entering an era of medicine where, for the first time, instead of just watching as patients lose basic abilities such as vision or movement, we can start to build devices that will help restore those abilities. What an exciting new time!
It is often the case that researchers can get discouraged by costly failures and uncertain obstacles, but this is the important work that serves as a necessary reminder that every once in a while, when things work out, it is actually possible to give someone back the gift of sight.
Citations:
Price, Jay. “Duke Fits First Patient in State History with ‘bionic Eye'”Newsobserver. N.p., 10 Sept. 2014. Web. 19 Oct. 2014.
http://www.newsobserver.com/2014/09/10/4140145/duke-fits-first-patient-in-state.html
Sugar Head
In 2003, Dr. Robert Lustig saw a six year old Latino boy in his clinic in Salinas, California. Juan weighed 100 pounds and was wider than he was tall, but his mother insisted he ate a healthy diet. When Dr. Lustig began to look more closely, Juan’s diet did seem ok for a growing boy; however, through his directed questions, Dr. Lustig found the somewhat unexpected culprit: orange juice. Juan had gotten into the habit of drinking an entire gallon of orange juice per day. This is approximately 1,760 calories and 336 grams of sugar, which is over 1 cup of sugar. Additionally, the amount of dietary fiber: 0 grams. Why was Juan doing this? Because the government provided it to his family for free, and his mother had no idea how harmful it could be to her son’s health. In fact, she felt that the more he drank, the more nutrients he was getting.
Although obesity has received a lot of media attention in the last few years, I was still floored by some of the statistics in Fed Up, a documentary I recently watched (and highly recommend). I was surprised that the focus was around the role sugar plays in the growing epidemic, a definite shift from the more common topics of saturated fat and exercise. The numbers get a little scary:
In the United States, it is estimated that 93 Million Americans are affected by obesity.
Kids watch an average of 4000 food-related ads every year (10/day).
A 20-ounce bottle of soda contains the equivalent of approximately 17 teaspoons of sugar.
It will take a 110-pound child 75 minutes of bike riding to burn off the calories in one 20-ounce bottle of soda.
In 2012, Americans consumed an average of 765 grams of sugar every 5 days, or 130 pounds each year.
We all know that the Western Diet, characterized by high saturated fat and refined sugar, has been implicated in a range of diseases such as type 2 diabetes, cardiovascular disease, and stroke, but do we know whether and how this diet is affecting our brain?
We start the quest for an answer to our question with a small neural structure called the hippocampus, named after the greek words hippos and kampos meaning “horse” and “sea monster” respectively. This is because of the structure’s unusual shape and appearance. Do you see the resemblance?
Much work has been done to try to understand this structure (and it happens to be the one that Henry Molaison had removed in the 1950’s-see About Gray Matters for more on this story). It is heavily implicated in memory, and more specifically, important for those memories involving spatial cues such as remembering how to navigate around your house. Because the hippocampus contains unusually large cells, it is particularly vulnerable to environmental insults, including things such as diet.
What protects the hippocampus from environmental toxins?
The blood brain barrier is a crucial component of the nervous system. It serves as a gate keeper who “decides” what unwanted components of the blood must stay out and which nutrients will be allowed in, protecting the brain from harmful substances.
If you think about a football stadium with entrances surrounding its periphery, the blood brain barrier would be like the people checking tickets. Only those with tickets would be allowed in. Now think about what might happen at the super bowl if many of those ticket checkers were just not there. People without tickets would start hopping over the barriers and entering the stadium to view the game for free. This is what happens when there is damage to the blood brain barrier: unwanted substances get into the brain.
So how does this answer our question about how Western Diet affects the brain?
Recent research has revealed two important trends:
1. Western Diets seem to stimulate intestinal production of a protein found in the body called amyloid-β.
2. Elevated levels of amyloid-β proteins have been shown to damage the blood brain barrier in rats.
Why does this matter?
One of the hallmark signs of a brain diseased by Alzheimer’s is the presence of plaques, particularly in the hippocampus. These plaques can be thought of as dangerous junk, cluttering the cell and disrupting normal function, and they are partially caused by the accumulation of amyloid-β proteins. Starting to see how this story is coming together?
Based on the current evidence, we can start to form a theory: A Western Diet increases bodily levels of amyloid-β protein, leading to increased amyloid-β levels in the blood. This elevation could contribute to blood brain barrier damage (equivalent to losing those ticket checkers!), resulting in more amyloid-β (ticketless individuals) being able to get into the brain. Once in the brain, these proteins can damage the large cells in the hippocampus, which are particularly vulnerable. The theory is laid out nicely in this diagram:
(1) Western Diet results in (2) elevated levels of amyloid-β (Aβ) from the small intestines, (3) thus increasing Aβ levels in the vascular system. (4) High levels of Aβ contribute to blood brain barrier damage, (5) which leaves the hippocampus (HPF) vulnerable to damage by Aβ.
So this leaves us with the possibility that obesity and dementia potentially share a common contributory factor: overconsumption of foods high in saturated fatty acids and simple sugars, or the Western Diet. Given the statistics about the prevalence of obesity in this country and others, the possibility that these people are also at a higher risk for future dementia is incredibly concerning.
Although not many people drink a gallon of juice every day, I have to admit that before reading Dr. Lustig’s book and watching Fed Up, I went out of my way to drink orange juice because I thought it was healthy for me. I did not realize how much sugar was in it! Now I just eat the fruit. I hope this will be better for my body and my brain in the long run.
For more information about the role sugar plays in the obesity epidemic, I recommend:
1. Fat Chance: The bitter truth about sugar by Robert Lustig
2. Fed Up Documentary (more information found here: http://fedupmovie.com/#/page/about-the-issue?scrollTo=facts)
Citations:
http://www.telegraph.co.uk/foodanddrink/10238549/Is-fruit-juice-bad-for-your-health.html
5 Crazy Ways Social Media Is Changing Your Brain Right Now
An interesting video from AsapSCIENCE about how social media affects the brain. Are we addicted?
Quick Review: Parkinson’s Disease
In 1817, a book called An Essay on the Shaking Palsy was published in which James Parkinson describes 6 patients who all demonstrated a similar collection of symptoms. He described the individuals as having increased tone in their muscles, slow and reduced movements, a stooped posture and a resting tremor. Decades later, famous french neurologist Jean-Martin Charcot coined the term “Parkinson’s Disease” and the description of the disease in medical textbooks remains much the same today (although additional symptoms involving altered cognitive abilities, problems with impulse control, sleep disturbance, vision abnormalities and others have also been included).
What do we know?
We know that in Parkinson’s Disease, cells that secrete the neurotransmitter dopamine in the depths of the brain die, affecting systems that control body movement, eye movements, emotional and cognitive functions. By the time someone starts to show motor symptoms, it is estimated that as many as 40-60% of these cells are already gone, and it is thought that the brain is able to compensate for their loss up until this point. Although scientists are still exploring the cause of this cell degeneration, one thing we do know is that when we look at these dopamine secreting cells from someone with Parkinson’s disease under a microscope, we can see what we call Lewy bodies. This is the brown blob seen inside the brain cell below. Lewy bodies can be thought of as junk and signal bad cell health.
What is not known?
Scientists are still working towards a complete understanding of Parkinson’s Disease. You may wonder how, if we have had a consistent description of the symptoms for hundreds of years, is there still so much that we don’t know. Take this example:
A few years ago, a 58 year old man, who had suffered from Parkinson’s for over 10 years, went to see Dr. Bastiaan Bloem in the Netherlands. This man’s brain had been ravaged by the disease and by the time Dr. Bloem saw him, he was barely able to walk on his own. When he tried to walk, often he froze in one place unable to even take a step or if he did, he could only take a few before falling over. But this man told Dr. Bloem something amazing, “Yesterday I rode my bicycle for 10 kilometers.” Dr. Bloem was in disbelief, and it was only after seeing it with his own eyes that he could start believing it.
Watch the video here: https://www.youtube.com/watch?v=aaY3gz5tJSk
It is still unknown why someone who is barely able to stand and walk on his own is able to smoothly ride a bicycle. Maybe the feedback the individual is getting from the pedals is allowing consistent movement initiation (something not present while walking) or perhaps riding is using a different part of the brain than walking. There have been reports of people with Parkinson’s Disease being able to dance, run, walk smoothly when given specific emotional or visual cues. It is still not clearly understood why this occurs, and more work is needed on how the motor system works to be able to explain these strange reports.
Are there treatments?
The most common treatment for Parkinson’s Disease is a drug that increases concentrations of dopamine in the nervous system called L-Dopa; however, more recently a surgery that implants an electrode into the depths of the brain has become more popular. This is called deep brain stimulation, and it has revolutionized treatment options for people diagnosed with Parkinson’s, especially those with early onset.
Check out this video that shows the amazing effects of deep brain stimulation for a patient with Parkinson’s Disease: https://www.youtube.com/watch?v=uBh2LxTW0s0
I have been absolutely fascinated by how well this surgery can work for some people and also the most important detail: neurosurgeons and neuroscientists still don’t really understand why placing an electrode in this one spot in the brain even has this effect!
This is just a very brief overview of some of the things I find most interesting about research on Parkinson’s Disease. There is a wealth of information out there, and some people spend their whole careers studying it. With the advancement of technology that allows us to sequence genes, stain cells, and image whole brains of living people suffering from this disease, we are inching closer to better treatments, and maybe even one day, a cure.
Citations:
http://en.wikipedia.org/wiki/History_of_Parkinson%27s_disease
http://www.nytimes.com/2010/04/01/health/01parkinsons.html?_r=0
Who me?
Imagine you are a young woman, feeling relieved that finally, at 3am, you are done with your shift at Ev’s Eleventh Hour Sports Bar in Queens, New York. You drive home to your city apartment building and park in the lot across the street. As you walk towards your door, you hear someone behind you. Your heart jumps into your throat as you see the man quickly approaching you. You start to run to a nearby intersection. Before you make it, you are stabbed twice in the back and scream out “Oh my god, he stabbed me! Help!” with all your remaining strength. A neighbor yells out “Let that girl alone!” and you think you are safe as your attacker runs away from you. You crawl towards your apartment door in search of help, but it’s locked. You lay there feeling weak and tired.
Unfortunately, this is the fate that met Catherine Genovese, the eldest of five children in a middle-class Italian American family from Brooklyn in March of 1964.
As she lay in the alley next to her building, Winston Moseley, her attacker, returned. He proceeded to stab her, rape her and then steal $50 before leaving her in a hallway. The whole attack spanned 30 minutes. Following the second attack, the police were called, but she died en route to the hospital. Later reports revealed that about a dozen people witnessed (in some way) a part of the attack including the man who had yelled out and scared Moseley away the first time. But if so many people heard her screams or saw her crawling in the street, why hadn’t anyone done something?
Did these neighbors not know what to do or did they just assume that someone else would call the police? One neighbor later admitted that they “didn’t want to get involved.”
This is a very famous incident that served as a key example of something known as the bystander effect. Social pyschologists have established that the presence of other people in a critical situation actually decreases the likelihood that someone will help. In their seminal work on the topic, John Darley and Bibb Latané, researchers at Columbia University, identified some possible explanations to explain this behavior.
1. Diffusion of responsibility: people tend to divide the responsibility by the number of bystanders. The more people there are, the less each individual will feel compelled to act.
2. Evaluation apprehension: people are fearful of others judging them while acting publicly. They are afraid that they will make a mistake or do the wrong thing with others watching.
3. Pluralistic ignorance: people tend to rely on others when navigating an ambiguous situation.
In a study carried out after Ginovese’s brutal attack, Darley and Latané wanted to see if this effect would play out in a laboratory setting. They recruited male Columbia University students with an ad for taking part in a survey about campus life. When they arrived at the experiment, they were shown into a room where they were told to fill out a preliminary questionnaire. While in this room, subjects were either:
1. alone
2. with two other subjects
or 3. with two researchers (pretending to be subjects).
While they were filling out the questionnaire, experimenters slowly introduced (harmless) smoke through a small vent in the wall. The smoke flowed in freely and after several minutes, it became so thick that vision was obscured. The researchers then watched behind a one-way window to see how the 3 groups would respond and to test whether those responses were different.
What do you think the results were?
When the subject was alone, he would typically see the smoke, get up and walk to the vent, sniff it, wave his hands in it, feel the temperature, and then after a short period, leave the room to look for someone to report it to. When the subject was in the room with two researchers who were instructed to behave indifferently to the smoke, only 1 in 10 reported it. The other 9 subjects remained in the room, determinedly working on their questionnaires, coughing and waving the smoke out of their eyes! In comparison to the response rate of the alone condition (75%), only 10% of subjects in this condition reported the smoke. Finally, when all 3 bystanders were naive, of the 24 people run in 8 groups, only 1 person reported the smoke within the first 4 minutes before the room became highly unpleasant!
Why does this happen?
In an exit interview, most subjects reported the smoke when asked if they experienced any difficulty with the questionnaire. They had all noticed it. Subjects who had reported the smoke during the experiment consistently reported that they thought it was “strange” and “it looked like something was wrong.” Subjects who had not reported the smoke during the experiment mainly all had decided that it was not a fire and had come up with some kind of alternative explanation for its presence. Some were convinced it was steam or a side-effect of the air conditioning unit. Two people even reported that they thought it was “truth gas” introduced to get them to answer the questions truthfully (the researchers report that they were shocked that these subjects did not seem disturbed at all by this belief).
Perhaps the subjects felt that having other people present increased their ability to cope with a fire. It is also possible that subjects in the group conditions aimed to appear more brave when others were watching; however, the researchers make a different argument. As they discovered in follow up interviews, it was not that subjects were unworried about the fire or willing to endure danger. It was that the subjects that did not report the smoke claimed that they had decided that there was no fire at all; the smoke was caused by a harmless source, a decision that was highly susceptible to social influence.
In the news reports of Catherine Genovese’s murder, reporters blamed the apathy that grips people who live in big cities. Darley and Latané conclude that the failure to intervene may be better explained by understanding the relationship among bystanders rather than that between a victim and a bystander.
I have always found this social psychology work fascinating and hugely informative and applicable to how I navigate the world. Knowing the traps and pitfalls that your brain can unknowingly fall victim to is the first step towards avoiding them. Here we see how the presence and behavior of others can influence an individual’s response in an emergency situation.
So, if you ever find yourself in an emergency situation (and I hope you don’t), try to remember the lessons we have learned from Catherine Genovese and think about whether or not you want to remain passive.
Citations:
http://listverse.com/2009/11/02/10-notorious-cases-of-the-bystander-effect/
http://en.wikipedia.org/wiki/Murder_of_Kitty_Genovese
http://psycnet.apa.org/journals/bul/137/4/517/
Click to access Group%20Inhibition.pdf